Abdominal Transplant Surgery
Abdominal Transplant Surgery
PROGRAM OVERVIEW
About the Program
The University of Washington Abdominal Transplant Surgery Fellowship is a two-year fellowship accredited by the American Society of Transplant Surgeons (ASTS). The program has been carefully designed to provide fellows with focused, hands-on training in Abdominal Transplant Surgery.
Throughout their training, fellows gain experience in:
- Operative techniques of deceased donor liver, kidney, and pancreas transplantation
- Operative techniques of living donor liver and kidney transplantation
- Deceased donor organ procurement (with a 20-30% rate of donation after circulatory death)
- Living donor hepatectomy and nephrectomy
- Fellows participate in the evaluation of donor offers
- Management and evaluation of transplant patients in the in and outpatient setting, including recipient and donor evaluations, post-operative management and management of immunosuppression and its complications
At the completion of this two-year program, fellows will be eligible for certification in liver and kidney transplantation. We are currently approved to match 3 fellows every two years. For the 2026 application cycle (with a fellowship start date of August 1, 2027) we have two open positions.
Program Leadership

Catherine Kling, MD MPH
Program Director,
Abdominal Transplant Fellowship
Assistant Professor, Transplant Surgery
Clinical Experience
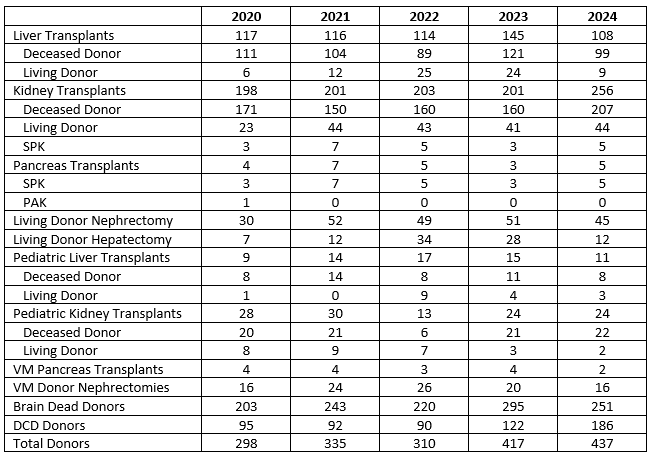
Our program aims to develop transplant surgeons who graduate with proficiency in all aspects of liver and kidney transplantation, deceased donor organ procurement, living donor nephrectomy, including pre- and post-operative management of the transplant patient, and operative independence. There is also additional experience in pediatric liver and kidney transplantation.
Training Sites
Throughout their two years of training, fellows will have the opportunity to rotate at three sites.
- The University of Washington Medical Center – Montlake is a tertiary and quaternary care referral site for the WWAMI region and serves as the primary training site for the Abdominal Transplant Fellowship.
- Seattle Children’s Hospital was founded over 100 years ago and serves families across the WWAMI region regardless of their ability to pay. Fellows will rotate here to gain experience in pediatric transplant surgery. (Located 2 miles west of UW Medical Center-Montlake)
- Virginia Mason Medical Center hosts a kidney and pancreas transplant program and is located 5 miles south of UW Medical Center-Montlake. Fellows rotate here to gain additional experience in pancreas transplantation and living donor nephrectomy. (Located 5 miles south of UW Medical Center-Montlake)
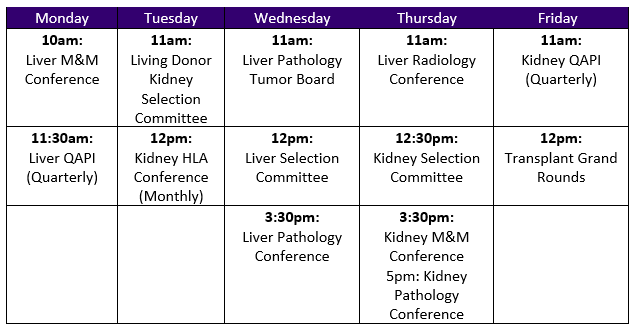
Conferences